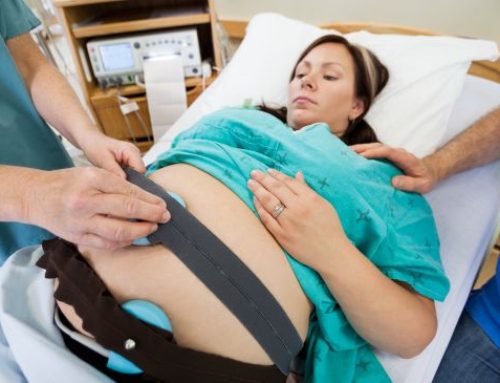
As we saw in our last article, food and water are being routinely withheld from seriously ill patients – not all of them terminally ill – in Canadian hospitals. Is this right? Can withdrawing nutrition (or failing to initiate it) ever be justified?
There are two major schools of thought on this matter, and two minor ones. To take the major ones first: – Those who would permit withdrawal argue that artificially provided nutrition is a medical treatment, like mechanical respiration, cardiac pulmonary resuscitation or drug therapy. When a treatment becomes inefficient, overly burdensome, or even results in the deterioration of the patient’s condition, it is no longer obligatory. – Those opposing withdrawal argue that providing food and water has always been considered basic human care, that this can be done without discomfort, and that refusing to do so would be equivalent to a sentence of death by starvation.
Two other opinions, less widely held, are that: – A patient has the right to refuse any ‘treatment’ – including nutrition. No one may force upon him a treatment he does not want. – In some cases it is permissible to withhold food and water. However, the common good demands that we not make exceptions to the general rule that nutrition constitutes basic human care, and must never be withdrawn.
There is no easy answer to the question, but the weight of human reason and of divine revelation seem to indicate a preference for this opinion.
Next month’s article will attempt to justify this choice.
However, before doing this it would be in order to ask where the major influence-groups stand on this issue: the Catholic Church, the medical associations, the doctors and other health care workers, the ethicists, the governments, the courts, and the media.
The Catholic Church
Although several popes have issued statements and published documents on treatment of the dying, no official pronouncement has been made. The Vatican clearly still has the matter under deliberation. The 1980 Declaration on Euthanasia contains statements which could support both sides of this issue. Individual bishops and regional Episcopal conferences have generally supported the pro-feeding position. The Canadian bishops have not issued a statement.
Catholic moral theologians have not yet reached a consensus either. In the 15th century, Antoninus believed that a sick person had the obligation to take reasonable measures to preserve his life, including obeying his doctor in matters of food and drink. In the 16th century, Vitoria limited this obligation to foods which were commonly available. In 1595, Banez introduced the terms ‘ordinary’ and ‘extraordinary’ means, thus providing a necessary distinction which has been helpful until recent times – although the definitions of these terms have had to keep pace with advancing medical technology.
In the 40’s and early 50’s, Gerald Kelly defined as ‘ordinary’ those means which “offer a reasonable hope of benefit and which can be obtained and used without excessive expense, pain or other inconvenience.”
A few years later, Daniel Cronin adjusted this slightly to include “those means commonly used in given circumstances, which this individual… can reasonably employ with definite hope of proportionate benefit.”
The word ‘proportionate’ has come to replace ‘ordinary’ in Catholic moral teaching and even in official Church documents; it was used in the 1980 Vatican Declaration on Euthanasia. During the last ten years, however, spurred largely by several notable U.S. court cases, Catholic moral theologians have divided into two camps: those who hold that providing nutrition is not always obligatory, and those who hold that it is. The former group includes Fathers Kelly, McCormick, Cronin, Paris, Farrahar, Moraclewski, O’Rouke, Varga, and Phlip Boyle (all Roman Catholic priests); while the latter includes Brown, Meilaender, Joseph Bole, and Frs. Barry, Callahan, Donovan, Connery and Smith.
Without getting into details about their respective arguments, it is fair to say that the pro-withholding theologians seem so far to have been more successful in linking their view with Catholic moral tradition. However, the pro-nutrition advocates have more clearly enunciated the dangers of failing to provide nutrition (dangers which their opponents often dismiss casually), and are supported by most of those bishops’ conferences which have taken a stand on the issue.
Medical Association
The Canadian Medical Association (CMA) has not yet taken a position. However, the Ontario Medical Association advises its doctors to “ start with the presumption that valid active care goals… may at any time include palliation… Treatment options are not routinely presented as an imperative.” Given the broad interpretation of the word ‘treatment,’ it is not difficult to anticipate an application to nutrition.
Outside Canada, the American Medical Association ruled in 1986 that nutrition and hydration may be withheld from a patient in an irreversible coma “even if death is not imminent.”
Doctors and other health-care workers
While statistics are not available, it is well known that many doctors and nurses approve of withholding nourishment, and in fact practice it. Some, with anonymity protected, have admitted doing so. The major factor is the desire or, in the absence of competence, the ‘best interests’ of the patient.
Some hospitals (e.g. Scarborough General in Toronto) have a policy against feeding patients as they approach death.
It is from the ‘rank and file’ health practitioners, in fact, that some of the most vigorous arguments in favour of withdrawals are originating. Joyce Zerwekh’s article on ‘The Dehydration Question’ has become a basic reference work in categorizing the medical dangers of tubal feeding. Dr. Stephen Cox of Tucson, Ariz., states that his experience with 4,000 patients who have died without intravenous (IV) support indicates that ‘terminal dehydration’ is not only a natural part of the dying process; it is not even painful.
Nevertheless, surveys of physicians have shown that 50-73% of them initiate IV therapy for dying comatose patients. Many doctors still believe, whatever the current trend may direct, that discontinuing IV therapy would break the link of trust binding their patients to them.
It should be noted, however, that no Canadian doctor has ever been convicted of killing his patient, despite doctors’ admissions that a nutrition withdrawal is routine, and the administering of lethal drug doses fairly common.
A 1983 survey of 300 Toronto-area doctors reported that 81% experience ethical problems in their daily practice. Despite this, only 1/3 had taken the Hippocratic oath, 2/3 of these did not know what it contained, and only a very few were familiar with key points in the CMA Code of Ethics.
Ethicists’ Guidance
The moral dilemmas caused by modern medical technology, and by the introduction of practices foreign to earlier generations of doctors, have created a demand for an ‘objective’ voice to guide medical practitioners in making difficult decisions. For this reason, ethicists are among the most influential people on the medical scene today.
Nearly all of them support the non-provision of nutrition in some cases. In addition to the hospital staff whose values they help clarify, many of them also teach medical ethics classes to medical students.
Few ethicists base their view on either divine or natural law. In fact, in the words of George Webster, clinical ethicist of St. Joseph’s Health Care System, in Toronto, “I work solely as an advisor… I raise questions and offer approaches to thinking that can sometimes clarify the issue and form a framework for addressing the problems.” This means, of course, that recommended actions will vary from team to team and from case to case.
An underlying absolute does seem to exist in the will of the patient. Since the ethicists operate in a world of relative goods, the ultimate value clarification is often what the patient wants, or is understood to want. Dr. William Harvey, ethics professor to several hundred medical students at Victoria College in Toronto, states categorically that the patient has the final decision about what happens to him. Since one of Dr. Harvey’s main complaints is that doctors do not know how to make ethical decisions, it can safely be assumed that his students will accept his doctrine of ultimate responsibility without being overly critical, and that many of our future doctors will base their ethical decisions on patient autonomy.
To interject a personal note – The strangest aspect of the ‘ethicist phenomenon’ is that, while many ethicists are familiar with Catholic moral tradition and are well-read in philosophy and contemporary medical and ethical literature, I have not met one or read any who believes in an absolute set of values whose truth is guaranteed by divine revelation or by right reason.
Government caution
As usual, government is being cautious, waiting for the people to speak. We saw last month that 75% of Canadians favour withdrawal of nutrition on demand. In 1983 the Law Reform Commission of Canada tabled a report stating that “any competent person should have the right to refuse treatment of any kind.” (The application of this principle to ‘starvation by election’ or to teen-age suicide must have been apparent to at least some senior government officials, because the report was not acted upon.)
However, increasing pressure from such groups as Dying with Dignity will almost certainly cause the Commission to introduce similar recommendation within a year or two. Dying with Dignity’s ultimate goal is the introduction of voluntary active euthanasia in Canada, so this will be simply a carefully planned step in that direction. Supported by ¾ of the voters, no government is likely to resist it.
Court decisions
Canadian courts have so far upheld the sanctity of human life, albeit shakily. In the 1983 Stephen Dawson case, a B.C. Supreme Court justice overturned a B.C. Family Court decision and ordered a life-saving brain shunt operation for 7-year-old Stephen. Ontario family courts have sometimes ordered operations to remove stomach blockage in newborn Down’s Syndrome infants. In no case involving care for the sick has a Canadian court ordered a course of action which by itself caused the death of a person after birth.
There is a possibility that one of the numerous nutrition-withdrawal cases mentioned earlier will find its way into the court system, and that the resulting decision may set the kind of unfortunate precedent which has already been set many times in the United States. Until then, however, the Canadian court system remains steadfast in its protection of the right to life after birth.
Media focus
The media have an agenda which is well known to every one with a Grade 5 education: sell subscriptions or air time by supporting the liberal (contemporary or progressive) side of any issue. No list of headlines needs to be given here; we have all seen enough to judge for ourselves. What the media will do is focus on the tragedy of allowing a severely handicapped child to die – because it ‘sells’ – while also making sure to mention the tragedy of allowing him to live. What the informed citizen expects of the media is self-interest – nothing more. There is no consensus in our religious or secular societies, therefore, concerning the provision of nutrition for the very ill. In this kind of vacuum, it is generally the less burdensome way which is chosen. But those who would allow the withholding of nourishment are ignoring three fundamental principles of human existence, principles which are among the foundation stones of western civilization, and without which it will surely fall. This will be the topic of next month’s article.